Is It Safe? Delayed doses, changing positions, and polypharmacy
More vaccine debate, experts getting things wrong, and guidelines that increase the pill burden.
If you find this post useful and think others might do so, spread the word.
Last week the UK was accused of abandoning science over mixing different COVID-19 vaccines as official policy (they had not, except in rare cases), and since Christmas there has been lots of discussion about the Joint Committee on Vaccine and Immunisations’ (JCVI) decision to delay the second dose of the Pfizer and Oxford AstraZeneca vaccine to maximise a quick roll of vaccine to at risk groups. I’m in the ‘this isn’t ideal, but this is a pandemic with a new easily transmissible variant that is causing a rising number of deaths’ or as Peter English has put it in a recent blogpost.
The bottom line is that delaying the second dose until 12 weeks (possibly longer) will prevent hospital admissions and save lives.
The other way of putting this is that not carrying out this policy will cause hospital admissions and lose lives.
I’m not going to repeat the material from this BMJ overview or the JVCI paper. But this short bit from the BMJ gets to the nub of the matter (my highlights).
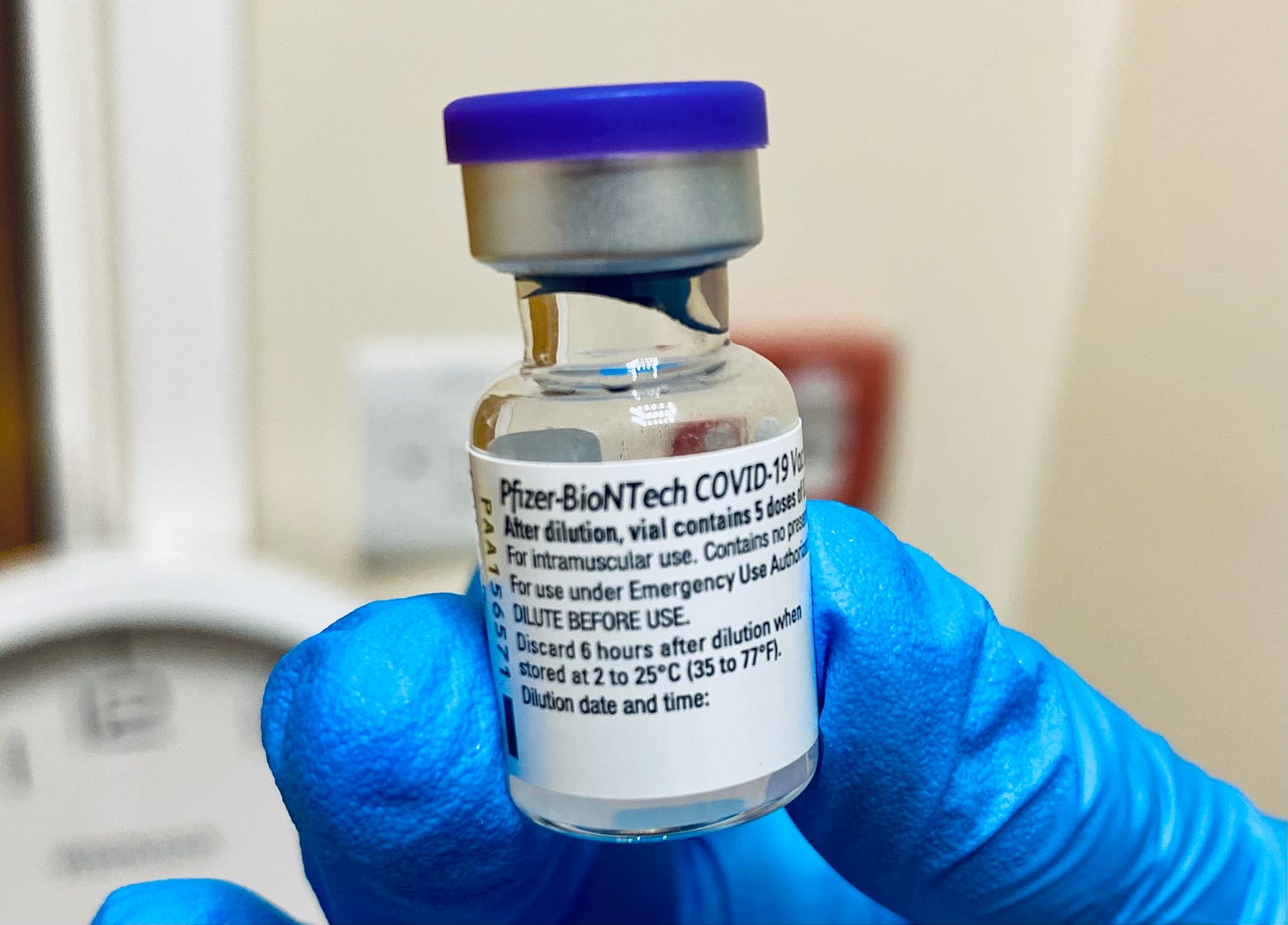
A paper published in the New England Journal of Medicine stated that the efficacy of the Pfizer-BioNTech vaccine was 52.4% between the first and second dose (spaced 21 days apart).5 However, in its “green book” Public Health England said that during the phase III trial most of the vaccine failures were in the days immediately after the first dose, indicating that the short term protection starts around day 10.6 Looking at the data from day 15 to 21, it calculated that the efficacy against symptomatic covid-19 was around 89% (95% confidence interval 52% to 97%). Meanwhile, Pfizer has said that it has no evidence that the protection lasts beyond the 21 days.
I still come across people stating the 52% figure, but this make little sense since that figure between the first and second vaccine stands whether you not you have the second dose delayed or not. The comparable figure is the 89%.
Tom Chivers, in a piece covering the vaccine mixing controversy, makes a good point about evidence.
You can understand the “no RCTs, no evidence” attitude. Over the last century or so, medicine has established a norm where the only evidence that really counts is lots of RCTs. There is an excellent reason for that: doctors’ intuition as to what worked and what didn’t was often extremely flawed, because doctors are people. So it is very important to show that your new drug or your surgical intervention does more good than harm before you introduce it.
But we simply can’t afford to wait for that level of certainty. Evidence, a wise man once said, is like money: “Obviously it’s useful to have as much evidence as possible, in the same way it’s useful to have as much money as possible. But equally obviously it’s useful to be able to use a limited amount of evidence wisely, in the same way it’s useful to be able to use a limited amount of money wisely.”
The other point about evidence based medicine is that it has never been about mindlessly sticking to randomised controlled trial evidence without context. One of the tiresome criticisms thrown at EBM is that it is too driven by data alone. Sackett et al defined it as ‘the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients.’ Changing ‘individual patient’ to ‘a population’ in a public health setting makes logical sense, and the JCVI appear to have been judicious in their use of the evidence in the face of rising deaths in the UK. The British Society for Immunology agrees.
In the end, I suspect second doses will be given, if delayed for some, and with luck the single dose Johnson & Johnson vaccine will make things even easier.
As an aside, there have been critics of the UK’s JCVI from people on the US equivalent of the JCVI:
"Bad idea," said Dr. Paul Offit, a member of the Food and Drug Administration's Vaccine Advisory Committee. "You're disrupting a program," he said, adding if a recipient's second dose is delayed "two months later, three months later, four months later ... they may not be protected anymore."
I’m not pulling out Offit to criticise him, he is an amazing vaccine advocate and scientist, but the moment I saw US criticism of the UK position, I started counting down how long it would be before they did something similar.
One of the surprising, and unhelpful, things that’s been happening since the vaccines started to appear is how insitutional voices in the EU and the US have been willing to make critical public statements about the UK regulator. In the EU, Peter Liese said their procedures were safer, which they have no evidence for. The UK regulator did a disproportionate amount of work for the EU, and they have not lost their expertise. This sort of behaviour does not seem helpful, especially in the sensitive area of vaccines, and in the age of a click-driven media who will headline the loudest disagreement.
There are always going to be differences in national responses, decisions, and timings, in part because decisions being made aren’t just about the vaccine, but also about factors such as disease prevalence. WHO recently was reported as being critical of the UK position, which led to twitter outrage about the UK, but Alejandro Cravioto, chairman of WHO’s Strategic Advisory Group of Experts on Immunization (SAGE) did say, “I think we have to be a bit open to these types of decisions which countries have to make according to their own epidemiological situations.”
I’ll also leave this here… (I haven’t got a view on the US regulator versus the UK regulator terms of forecasting, but the question and the quoted tweet thread underneath is interesting.)


This could be evidenced by the decision of the FDA not to grant a licence to the Oxford Astra-Zeneca vaccine, and letting a vaccine plant stay idle in the face of a pandemic.
Changing positions and uncertainty…
There will probably be lessons to learn about how to communicate messaging to both the public and professionals about changes to vaccine policy, since it does lead to concern that things are just being done on the hoof, even if options are being carefully evaluated by experts. Still is it preferable that decisions are made in the face of changing evidence and circumstances. Perhaps one thing we need the public to understand, more than ever, is that science and judgments have to change. Part of that might be experts being a lot less certain about their views in the first place.
I was reminded this week of a BBC Radio 4 Briefing Room episode “How dangerous is the coronavirus” I had listened to back in January 23rd 2020 when COVID-19 was only just appearing in the public consciousness. It is quite remarkable to listen to now. (It is only on the BBC site for a further 13 days).


One of the experts in this programme is currently telling people the UK could vaccinate the entire population in 5 days. He’s a better academic than I will ever be, but sometimes clever people can be very wrong. And this is worth watching, via Ian Leslie who wrote a good piece on experts.

Polypharmacy and older people
A colleague has a comment piece out on the burden of medicines in older people, which is worth reading, but this was the stand out part in my view.
Practitioners face a challenge in managing several chronic conditions using clinical guidelines that predominantly focus on single disease, not always considering the presence of any co‐morbidity. Potentially, a hypothetical 78‐year‐old woman with past medical history of myocardial infarction, type 2 diabetes, osteoarthritis, chronic obstructive pulmonary disease and depression could be the subject of five UK clinical guidelines, and take a minimum of 11 prescribed medications, increasing to 21 medications as her various diseases progress.
Guidelines are, well, they are guidelines. They aren’t rules. Individual prescribers need to look at the overall picture in a patient before adding an additional medication burden upon them. Any incentives for compliance with guidelines at an organisational level need to be aware of this counterproductive side effect of guidelines.
Stay safe.
Anthony
Don’t forget to report your suspected adverse effects from medicines and vaccines. In the UK, this means using the Yellow Card Scheme